Key Takeaways
High denial rates are the top back-end RCM problem. 40% of LHS listed high denials rates as their biggest challenge for back-end revenue cycle management—the top response of all options.
Denials management is becoming more time-consuming and staff intensive. 73% of LHS surveyed have more than 60+ full-time employees (FTE) on their revenue cycle team, while nearly 60% spend at least 30% of their time on denials management.
LHS are trying to be more proactive to get ahead of the problem. The good news: 83% of LHS are confident they know which denials are likely to be overturned. “Request for Additional Documentation” denials have the highest success rate with 88% of appeals being successful. Therefore, many are looking to automate these proactively.
Automation is still early. However, automation is still in the early stages for many. Nearly 70% of LHS surveyed have less than a quarter of their denials managed using automation.
Introduction
The Health Management Academy (THMA) in partnership with Finvi set out to understand how Leading Health Systems (LHS) approach denials management and how they make strategic decisions to invest in technology to transform the back-end revenue cycle. LHS are defined as innovative integrated delivery systems with over $2 billion in total operating revenue. This research captures perspectives from 5 qualitative interviews and 30 survey respondents, representing a significant share of the Leading Health System market.

Denials Remain a Key Part of RCM Optimization
Faced with the dual challenges of tighter margins and rising costs, LHS are under intense pressure to optimize their revenue cycle management (RCM) to capture every dollar, and a key component to that work is denials management. Denials management plays a pivotal role in RCM optimization due to its direct impact on financial health and operational efficiency. By effectively managing denials, LHS can minimize revenue leakage and enhance cash flow, ensuring a steady stream of income crucial for sustaining operations and investing in quality patient care. According to a 2022 study, unresolved claims denials represent an average annual loss of $5 million for hospitals, which results in up to 5% of net patient revenue.
Given the sizable impact of denials management, LHS expend considerable time and energy to improve workflows, communication, and technology that address the issue. Denials often result from errors in coding, incomplete documentation, or misunderstandings of payer requirements. As a result, implementing robust denials management processes allows LHS to identify root causes, address underlying issues, and implement corrective measures to prevent future denials. This proactive approach not only improves revenue capture but also streamlines workflows, reducing administrative burden and enhancing staff productivity.
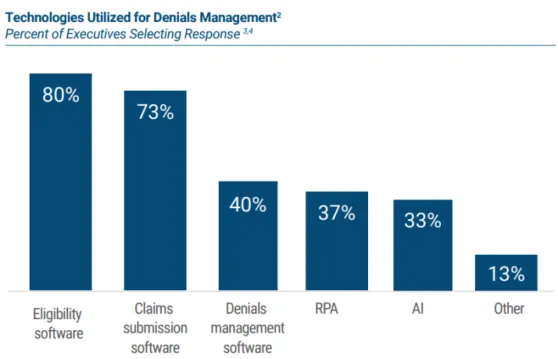
However, due to LHS’s complex RCM needs, especially for denials and back-end support, they turn to assistance from third-party support or external partnerships. Revenue cycle partnerships can provide dedicated support for the back-end of the revenue cycle and allow RCM leaders to focus their time and energy on more critical RCM optimization projects. LHS surveyed identified eligibility software and claims submission software as the top two most utilized software for denials management at 80% and 73%, respectively.
Key Lessons on Denials Management from LHS
1. Return on investment drives RCM partnership considerations.
The top factor for LHS when considering an RCM partner for denials management is the ability to demonstrate significant return on investment (ROI). LHS prioritize partnerships that offer tangible financial benefits, such as increased revenue capture, reduced operating costs, and improved efficiency. By ensuring a strong ROI, health systems can justify investments in partnerships, aligning with their overarching goal of delivering high-quality care while maintaining financial viability in a competitive healthcare landscape.
2. Denials management is early in automation maturity, but LHS remain open.
Despite nearly 70% of LHS surveyed having less than a quarter of their denials managed using automation, highlighting the minimal investment in automation so far, LHS do see the potential in new technology solutions. LHS seek an RCM partner who has advanced technology and automation capabilities to optimize their revenue cycle functions, improve efficiency, and guide them through technology advancements.
3. Payer relationships are a major area for improvement.
Both quantitative and qualitative data showcase how payers continue to influence how care is delivered and LHS capture revenue. For denials management specifically, payer relationships are paramount and prospective RCM partners should have a comprehensive understanding of the motivations of both payers and LHS to adequately improve denial rates, encourage proactive appeals, and increase revenue.
